
Looking Back at Alyson Stover’s AOTA Presidency and the Future of Occupational Therapy
For over 20 years, Alyson Stover has been a skilled occupational therapist, gaining valuable knowledge about the field of occupational therapy and applying it to her work in the classroom as an associate professor in Pitt’s Department of Occupational Therapy. Stover expanded her leadership experience with her recent position as president of the American Occupational Therapy Association.
Read More
Hear From the Director: What Makes the Pitt Master of Rehabilitation Technology Program Stand Out
Master of Rehabilitation Technology Program Director Julie Faieta shares what makes the program stand out.
Read More
Pitt Research Team Launches Consumer-Focused OTC Hearing Aid Dashboard
The CLEARdashboard interface alleviates uncertainty by guiding the user through a series of questions to filter different OTC hearing aids on the market to find the best solution for their needs.
Read More
From Class to Top Conference Award: Pitt Sports Science Alumna Desiree George
She not only gained confidence and experience being a sports and conditioning coach, but also in presenting research, which earned her the top award at the National Strength and Conditioning Association National Conference in July.
Read More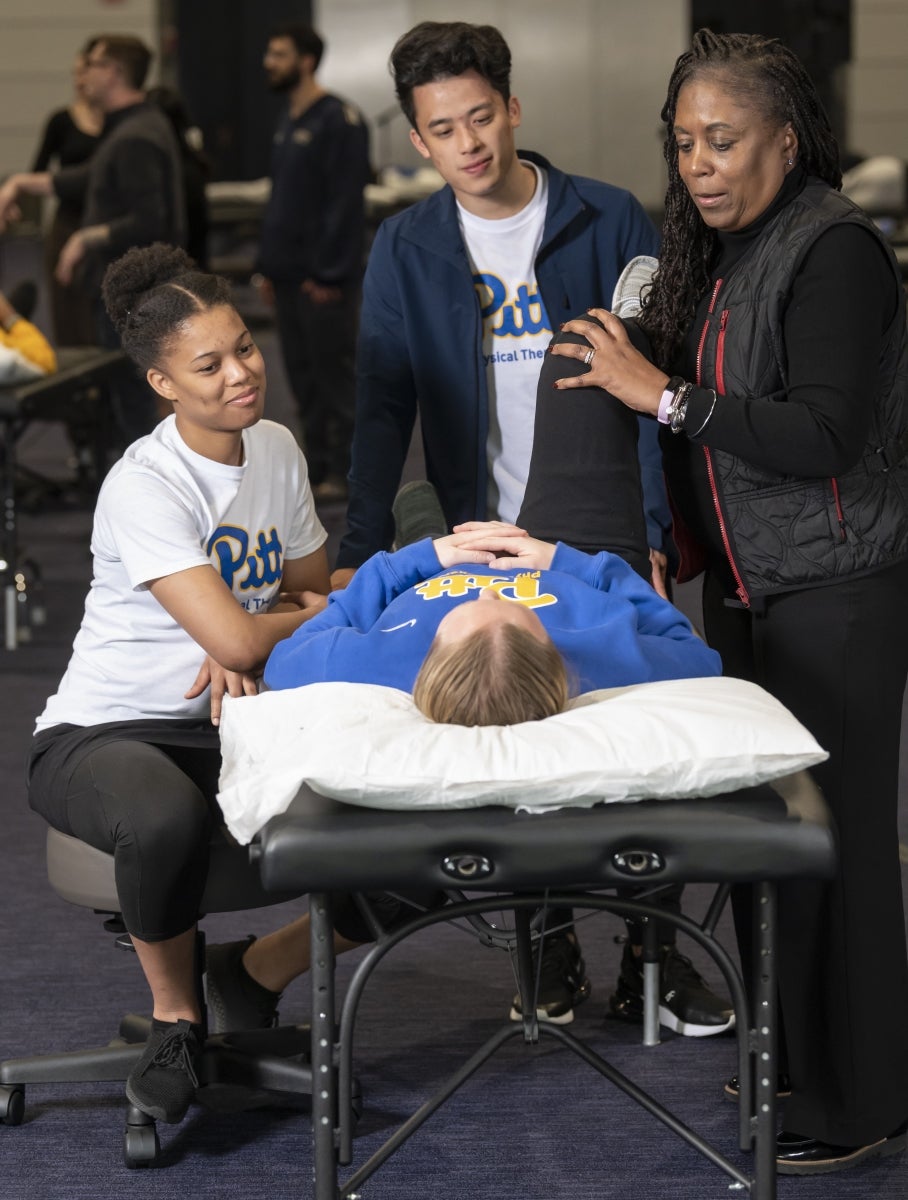
How to Become a Physical Therapist in 6 Steps
Are you looking to have a profound effect on people’s lives through improving their mobility and function? A career as a physical therapist could be for you! Our experts at Pitt PT give you all the insight on the steps needed to join the profession.
Read MoreLatest Stories
SHRS in the News
-
-
-
-
November 14, 2025 | Pittsburgh Post-Gazette | James Katz, Elaine Mormer, Catherine Palmer, Aravind Parthasarathy
-


